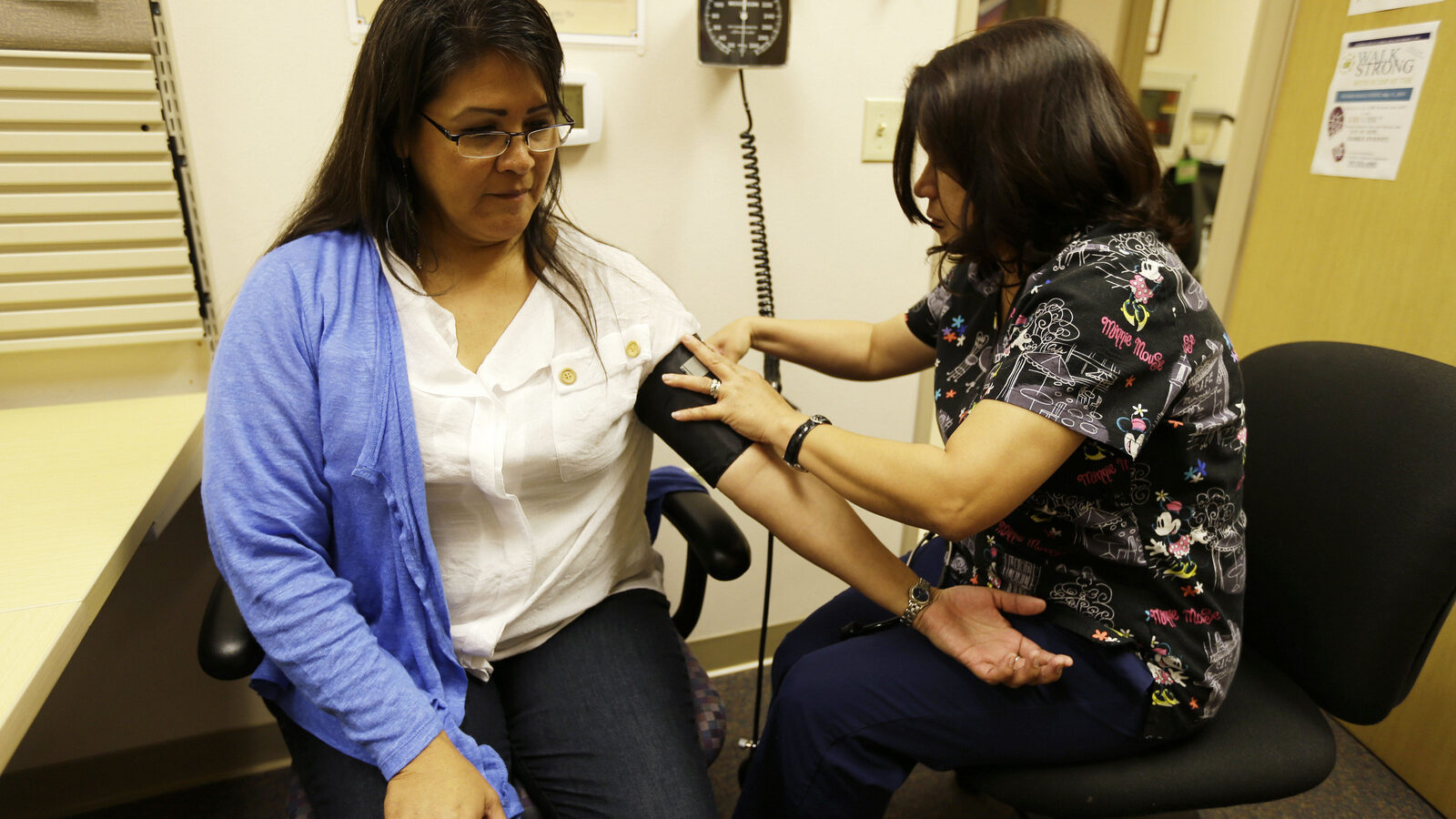The Indian Health Service (IHS), the federal service legally responsible for providing medical care to approximately 2.2. million tribal members is under scrutiny for failing to meet minimum national standards for medical facilities and repeatedly endangering patients by turning away the gravely ill and causing unnecessary deaths.
A unit of the Department of Health and Human Services, the IHS is similar in structure to the also dysfunctional Veterans Health Administration, as it operates a network of hospitals and clinics that provide medical services to tribal members who often live hours from other such facilities and lack private health insurance.
Despite the hundreds of federal investigations into claims of medical malpractice and employee misconduct, little has changed at the IHS as scandals continue to mount, with the system itself approaching collapse.
Problematic issues for the embattled health service are expected to get even worse due to cuts requested by the Trump administration in its IHS budget proposal, which would cut funding by $300 million.
A recent Senate hearing sought to shed light on the likely effects of the cuts, but acting IHS Director Michael Weahkee infuriated several Congressmen by refusing to answer basic questions. “I cannot believe what has transpired today. All I want is some damn answers, that’s it,” said Sen. Jon Tester (D-MT) after the Senate hearing.
Tester, Murkowski infuriated by Indian Health Service response to proposed cuts https://t.co/6K1kRAijSh via @missoulian
— Bart Mihailovich (@BartMihailovich) July 13, 2017
A lack of funds is one of the several major issues facing the service. In 2013, the IHS spent $2,849 per patient – significantly less than the national average that same year of $7,535 per patient and Medicare’s $12,042 per patient. IHS facilities often run out of funds before the end of the fiscal year. “A lot of tribes used to say, ‘Don’t get sick after June,’ ” Danette Ives, health director of the Port Gamble Tribe, told the Seattle Post-Intelligencer. “Now it’s like, ‘Don’t get sick after January.’ “
However, underfunding at the IHS is just the tip of the iceberg. As the Wall Street Journal reported last Friday, misdiagnoses and medical malpractice are unfortunate realities for those seeking treatment at IHS facilities, causing many tribal members to fear using the service, despite it being the only nearby or affordable option.
Many of the examples given by families of malpractice victims and recorded in official documents are startling. For instance, Wakanda Gonsalves, a high school senior from South Dakota, went to an IHS clinic to seek treatment after she began coughing up blood. She was sent home that same day with cough syrup, an inhaler, and anti-anxiety medication, only to die two days later from a blood clot in her lung.
Another native woman, Debra Free of Nebraska, died of an apparent opioid overdose at the IHS hospital in Winnebago ten hours after nurses ignored the orders of two doctors to stop treating Free with powerful narcotics. The Winnebago hospital has repeatedly failed to meet basic medical facility standards and has been found to have put patients in danger numerous times since 2010, according to U.S. hospital regulators cited by the Journal.
A prom queen was coughing up blood. An Indian Health Service doctor gave her cough syrup and antianxiety medication.https://t.co/v71BcjnG9e
— The Wall Street Journal (@WSJ) July 7, 2017
The Wall Street Journal also noted that IHS staff are often ridiculed or pressured to remain silent if they voice concerns about patient treatment or avoidable deaths to superiors or regulators. However, the IHS maintains that its “leadership maintains a culture where employees are encouraged and expected to report any reasonable suspicion of wrongdoing, misconduct, waste, or abuse, particularly when it involves the safety and well-being of patients or employees.”
Given the sorry state of the IHS, it is not surprising that those living on many tribal reservations have some of the lowest life expectancy rates in the entire nation. Native Americans have experienced jumps in mortality rates, including infant mortality, while those figures have decreased for other Americans.
Feature photo | Liz DeRouen, 49, left, gets her blood pressure checked by medical assistant Jacklyn Stra, right, at the Sonoma County Indian Health Project in Santa Rosa, Calif. Eric Risberg | AP