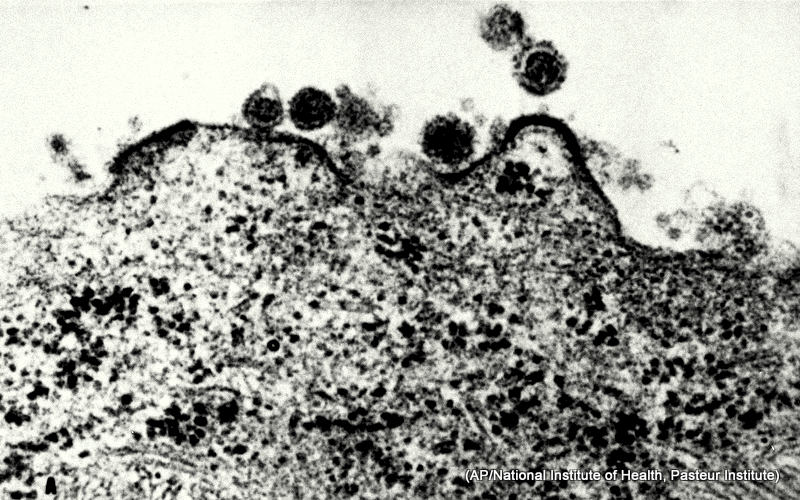
Eighteen months ago, a then-two-year-old child offered the first true glimmer of hope in eradicating HIV in children.
Following an abnormal and accelerated treatment regimen in which the baby — who had not been diagnosed with HIV at the time, but was suspected of carrying the virus because her mother had been HIV-positive during the pregnancy — was subjected to a three-drug antiviral infusion within 30 hours of birth, the child appeared to be HIV-free.
This represented the first case of an HIV patient being “cured” without the use of a blood transfusion or bone marrow donation. The “cure,” however, was not what it seemed: the virus was detected in the child’s bloodstream this month.
“Certainly, this is a disappointing turn of events for this young child, the medical staff involved in the child’s care, and the HIV/AIDS research community,” said Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, in a July 10 statement. “Scientifically, this development reminds us that we still have much more to learn about the intricacies of HIV infection and where the virus hides in the body. The [National Institutes of Health] remains committed to moving forward with research on a cure for HIV infection.”
The child, known in clinical circles as “the Mississippi Baby,” was born premature in 2010 to an HIV-positive mother who did not take antiretroviral medications during the pregnancy. Suspecting a high possibility of infection in the infant, pediatricians at the University of Mississippi Medical Center in Jackson, led by HIV specialist Dr. Hannah Gay, took the extraordinary step of putting the newborn on a liquid infusion to help prevent the contraction of HIV. The virus was detected two days after the infusion started, but treatment would continue for the next 18 months.
Around that time, the child’s mother stopped bringing the child in for treatment. Five months later, the child was returned for treatment, and upon testing her blood, no significant quantity of HIV was detected. HIV is thought to manifest in the human body by creating “reservoir” of viral material within infected cells. As these “reservoirs” are within the cells themselves, the body’s natural defenses cannot apprehend or destroy them and medicinal treatments cannot eliminate them — antiviral and antiretroviral treatments can only slow the development of new reservoirs. These “reservoirs” can sit latent for years. In the case of “the Mississippi Baby,” it was thought that the early, aggressive treatment wiped out the virus before the “reservoirs” could be created.
AIDS is actually an advanced phase in the HIV infection, in which the concentration of the virus in the body has reached a concentration that the virus is actively destroying T helper cells — cells essential for the functionality of the adaptive immune system. Without these cells, the body’s antibody and phagocytic responses are limited, leaving the body prone to opportunistic diseases such as lymphoma, cervical cancer and Kaposi’s sarcoma.
It would seem now that the virus continued to exist in the baby’s body, though in minute concentrations. In the absence of treatment, the virus started to multiply again and eventually formed “reservoirs.” Yet researchers feel that while “the Mississippi Baby” case proved not to be the cure they sought, it does offer hope for effective treatments toward long-term suppression of the virus.
“The fact that this child was able to remain off antiretroviral treatment for two years and maintain quiescent virus for that length of time is unprecedented,” said Deborah Persaud, professor of infectious diseases at the John Hopkins Children’s Center in Baltimore. “Typically, when treatment is stopped, HIV levels rebound within weeks, not years.”
Even though HIV infections have dropped by a third in the United States in the last decade, the infection rate remains high in Africa and among homosexual and bisexual men. While the 2007 case Timothy Ray Brown — also known as “The Berlin Patient,” he effectively became HIV-free after receiving a bone marrow transplant from an HIV-resistant donor — shows that the HIV infection can be effectively eliminated through surgical enhancement of the immune system, the need for a non-surgical, easily-administered cure remains pertinent.
In May, the Centers for Disease Control and Prevention released findings suggesting that individuals at high risk of contracting HIV should take HIV suppression medications, even if the individual is not currently HIV-positive. This approach, known as pre-exposure prophylaxis, or PREP, has been shown to reduce HIV infection rates by as much as 90 percent. While the prospects of an HIV vaccine are thin due to the fact that there have been no reported incidents of an individual developing the antibodies to fight the virus naturally and because even weakened HIV has the potential to cause infection, the use of PREP — as demonstrated in “the Mississippi Baby” case — may offer the best opportunity toward ending the HIV/AIDS pandemic.
However, with many seeing being HIV-positive as a stigma and opting not to be tested or to disclose their infections, HIV/AIDS remains a spreading global pandemic. With the recent loss of dozens of HIV/AIDS researchers in the attack on Malaysia Airlines Flight 17 — including Joep Lange, who pioneered the early antiretroviral trials and studied the transmission of the virus in vitro — the continued need toward research of the virus is just as essential as ever. However, truly controlling this virus may require a commitment to education and public support for those who may be fighting infection alone.
“Some people, if they find out they’re HIV-positive, they will change hospitals or scratch out their test result on their medical records,”

