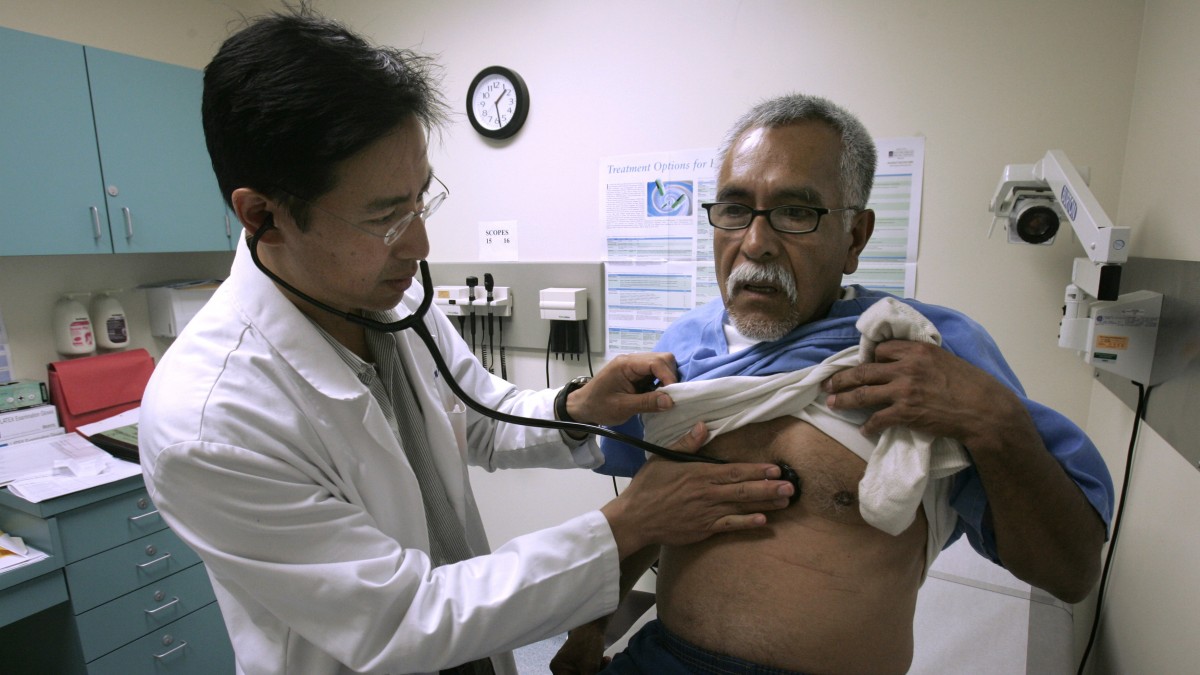
(NEW YORK) MintPress — If you are in need of emergency medical treatment, California is not the place to be. Especially if you are a member of a minority group. A new study has found that hospitals serving large minority populations were more likely to divert ambulances to other hospitals.
The study by UC San Francisco, Stanford University and UCLA measured overcrowding in 202 California emergency rooms. Scores of California hospitals have shut down their emergency rooms or closed entirely in the last decade, leading to long waits, diverted ambulances and, in the most extreme cases, patient deaths.
The closures also mean that patients in need of emergency care may need to travel farther, delaying access to treatment.
According to the American College of Emergency Physicians (ACEP), California has 7.1 emergency departments per 1 million people, compared to an average of 19.9 among other states, and the wait time is 27 minutes longer than the national average.
The findings of the study “are a matter of concern given that ambulance diversion has been associated with poorer health outcomes,” researchers said.
Disproportionate care
Hospitals serving large minority populations may be more crowded because there are fewer hospitals in their communities. “People think sometimes that there is a government body that has oversight of the supply and demand of emergency department care and that there is a rational system in place,” said Renee Hsia, the lead author of the study and an assistant professor of emergency medicine at UC San Francisco.
“But that’s not how the health care system works; it’s market driven,” she acknowledged. “The emergency departments in some communities tend to be cost centers because they serve uninsured patients and some are revenue centers because they are bringing in paying patients.”
Organizations like the California Hospital Association contend that hospitals are also overcrowded because some patients don’t have access to preventive and primary care.
Nonelderly minorities in California are less likely than whites to have health insurance, according to the Henry J. Kaiser Family Foundation, and researchers noted that they are also more likely to use emergency rooms for safety net care.
“The reason minorities use the emergency department more can be attributed to the fact that they can’t find a primary care physician to see them,” said Ellis Weeker, vice president of ACEP and a practicing emergency department doctor in San Jose. “The real issue is there needs to be places for people to go with their primary care needs – that’s what this is about.”
Difficult decision
In California, ambulance diversion policies are drafted by the 31 local emergency management agencies. Some hospitals use software programs to track the volume of emergency department patients in their area.
Determining when to implement an ambulance diversion is complicated and controversial. According to a policy brief issued by the California HealthCare Foundation in 2009, diversions are “unhealthy for the patient from the standpoint of quality, outcome and length of stay. It is unhealthy for the community because it delivers patients to a hospital that may not be the best fit for their individual and immediate needs.”
In addition, said Hsia of UC San Francisco, even though minorities tended to be most affected by ambulance diversion, it’s an issue that has ripple effects on all patients.
“What ends up happening is if your hospital goes into diversion, it affects other hospitals and it’s like a domino effect,” she explained. “The effects are not just on patients in the emergency department; it’s on people waiting for an ambulance that might be out of commission because it is circling the city (to get to a hospital that will accept the patient). The overall effects are felt by everybody.”
Poor prognosis
Some experts, like Rand Corporation researcher Dr. Arthur L. Kellermann, maintain that hospitals need to run more efficiently and move patients through the system more quickly.
The new study concluded that “system-level policies whether at the hospital or county level regulating ambulance diversion may help policy makers, health care providers and hospital administrators reduce diversion and its associated inequalities.”
Some states have taken more drastic measures. New Hampshire and Massachusetts, for example, do not allow hospitals to divert ambulances at all.
Whatever solutions California considers, it’s clear that its emergency medical care system is in need of a lifeline.